“You’re going to need to do some homework,” she said.
It was my first week of working at Youth on Fire (YOF), a drop in center and HIV prevention program for 14-24 year olds experiencing homelessness and housing instability.
“Okay,” I replied, expecting to be given some books or articles to read.
“I want you to go home, stand in front of a mirror, and say the words ‘blow job’ and ‘anal sex’ thirty times per day for the next week.”
“What?” I asked, certain that I had misheard my new supervisor’s instructions.
“You heard me correctly,” she replied. “I need you to practice saying ‘blow job’ and ‘anal sex’ until you can do it without blushing.”
“Ummm…” I said quizzically, blushing deeply.
She looked directly into my eyes. “We work with young people who are doing sex work. And who are having anal sex. We are an HIV prevention program – which means that we need to be able to talk about sex and sexual behavior without fear, shame, or judgment.” She paused and looked at me again. “If you keep blushing like this, no one is ever going to talk to you about what they do. And, if you can’t talk to them about how they have sex, you can’t effectively talk to them about how to prevent HIV.”
Until that moment, no one had ever talked to me about how to talk about sex. For that matter, I don’t think that anyone had actually ever talked to me about sex – beyond references to reputation and consequences. Most Americans grow up in a culture where we do not discuss sex, sexual pleasure, or sexual scenarios. Conversations about sex most often center on issues of consent, pregnancy, and disease prevention. We have been described as “Permissive Puritans” – people who are too uptight to comfortably discuss the behaviors in which we engage.
Soon after I began working at YOF (and practiced my phrases in the mirror), we revised our intake from only collecting basic demographic information to providing a thorough risk assessment. We began asking about housing history, substance use, and sex. As we refined our tool, we realized that to get useful information, we had to ask the right questions. Instead of “How many partners do you have?” and “Do you use condoms?” we began asking these questions: “Have you had oral sex? Vaginal sex? Anal sex?” “Have your partners been men, women, or trans folks?” “What influences your decisions to use condoms or not? Is it connected to substance use? Is it about the relationship you have with your partner? Does it depend on the availability of a condom?” When we asked these questions and listened to the answers without shock or judgment, we were able to engage in informative and meaningful conversations about sex and sexual risk and do HIV prevention based in our clients’ reality. Read Ayala's tips for dealing with frustration and heartbreak while supporting clients.
June 27 is National HIV testing day. While the rates of HIV infection have decreased in some communities, there are communities in which the rates are alarmingly high. Estimates suggest if current HIV diagnoses rates persist, 50 percent of men who have sex with men (MSM) of color will be diagnosed with HIV in their lifetime. Women of color make up 80 percent of new HIV diagnoses among women. And research suggests that 44 percent of youth aged 18 to 24 years who are HIV positive do not know their status. If we want to reduce the rates of HIV infection, we must talk openly and honestly with people about their risks and ensure they are getting tested regularly.
Here are some suggestions for providers who want to become more comfortable talking about sex with clients:
1. Practice, Practice, Practice.
In the adult education world, there is a concept called the “Conscious Competence Matrix."
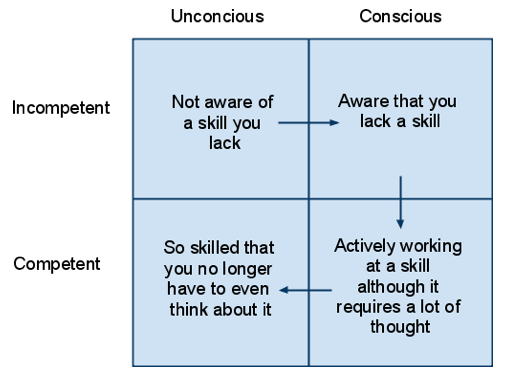
The basic concept is that we are all “unconsciously incompetent” when we don’t know that we are lacking a skill. We then move to “conscious incompetence” where we are aware (often acutely) of our lack of skill. Hopefully, we continue to develop our skills, and we then move to “conscious competence,” where we can do things well, but still need to think about them. Finally, the last stage is “unconscious competence,” where the skills are part of our repertoire, and we no longer have to think about them or intentionally implement them – it just becomes part of who we are and how we operate. Eventually, I didn’t have to think about when and how to ask about sex. I just did it naturally and instinctively.
2. Explore your own hang-ups.
Part of the burden of being human (rather than a robot) is that we have judgments and reactions to things. The task is not to rid ourselves of these reactions, but rather to know them and be aware of how they impact and influence our interactions with clients. This may mean digging into your own homo- or trans-phobia or discomfort with BDSM (bondage, domination, and sadomasochism) practices. It may mean facing your unease and upbringing. It may mean some uncomfortable conversations and realizations. However, it is necessary to do this self-exploration to provide effective HIV prevention.
3. Understand Harm Reduction and the sexual risk continuum.
Not all sexual behaviors carry the same risk for HIV or sexually transmitted infection (STI) transmission. And even if someone is going to engage in behavior that carries high risk of transmission (e.g. unprotected receptive anal sex), there are many ways that the risk of transmission can be reduced IN ADDITION to using a condom. For example, water-based lubricant reduces risk of tearing and therefore reduces risk of infection, even in the absence of a condom. In Harm Reduction, there is a phrase “the optimal outcome is not the only outcome” – ideally people will engage in behaviors that put them at the lowest risk of negative outcomes. And, at the same time, there are always small steps people can take to move them in the direction of health and wellness. Every step in that direction is a victory.
4. Be curious and humble.
If we can stay curious about our clients and humble about our own limitations, we set the stage for a collaborative partnership with clients, where we can support them in understanding their values and behaviors and adapt their behaviors accordingly.
I am grateful to my mentors, teachers, and clients who have taught me so much about how to do effective HIV prevention work. I hope that in honor of HIV Testing Day, everyone who works with vulnerable clients will make a commitment to increase their comfort talking about sex and sexual behaviors. Imagine what might happen if we could all talk about sex without fear, judgment, or shame. Or even just without blushing!
Hear more from Ayala by listening to a t3 podcast: "Beyond Tokenism: The Power of Lived Experience"
For HIV/AIDS resources from the Center for Social Innovation's Praxis project, click here.
Images from top to bottom by Wheeler Cowperthwaite (cc by 2.0) & pgbailey (cc by 2.0).








